Focus On Nursing
Focus On Nursing: A High Demand, High Growth Job of the Future
If you’re looking for a job in the future, then nursing is one of the strongest candidates out there. Although some aspects of the role may be susceptible to automation—in Japan scientists have developed a robot that can hand out medication and collect records—the central importance of empathy and advanced motor skills to nursing jobs makes it highly unlikely that machines will be replacing humans at our bedsides any time soon.
But that’s not all: According to the 2014 U.S. Census Bureau report, by 2050, the number of U.S. residents aged 65 and over is projected to be 83.7 million. As the population ages, there will be ever greater demand for healthcare professionals of all stripes, including nurses. And unlike many other fast-growing “jobs of the future,” the doors of a nursing career are open to those without a college degree.
But there’s a flip side, one that’s all too familiar to employers. As demand for nurses rises, the supply of qualified candidates does not always keep up, with the result that the U.S. faces a nursing shortage. So what is to be done? To get a deeper insight into the situation, we spoke with Dr. Joyce Knestrick, president of the American Association of Nurse Practitioners and an Associate Professor of Nursing at Georgetown University.
Although it’s a convenient shorthand to talk about “nursing,” the reality is that this is a rich and diverse field.
“That’s one thing I love about the nursing role—that there are so many different opportunities,” says Dr. Knestrick. “I think younger people aren’t necessarily aware of all of the opportunities within the field,” she adds.
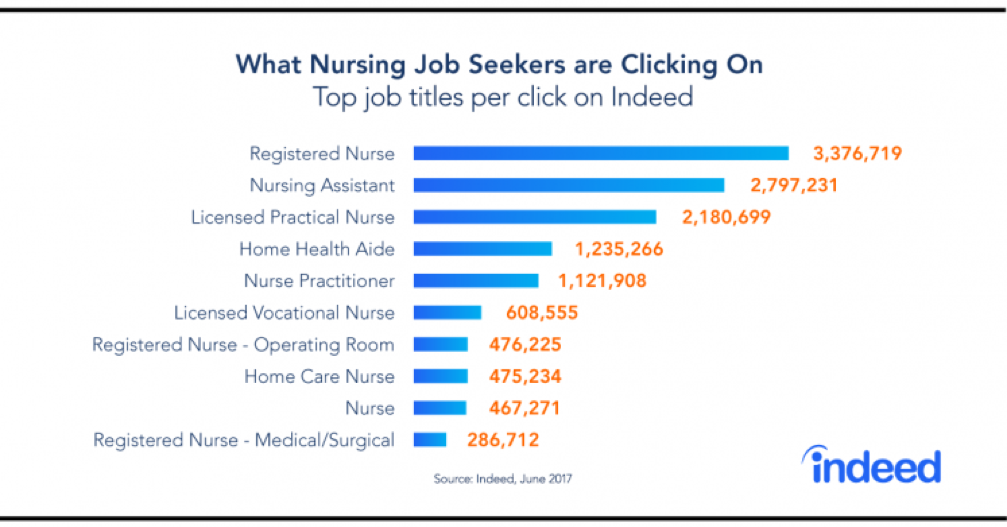
Thus, while demand is high for registered nurse (RN) roles (projected to see an impressive 16% growth through 2024, according to the BLS) there are many possible specializations.
For instance, Dr. Knestrick cites roles in management, nursing administration and nurse practitioner roles (these are nurses with an advanced degree who combine clinical diagnostic and treatment expertise with an emphasis on illness prevention). Then there are pediatric, neonatal, psychiatric, mental specialists and women’s health nurse practitioners.
And this is not to mention the nurse anesthetists, nurse midwives or people working in nursing informatics, who combine health science, computer science and IT skills to manage large amounts of patient care data. The possibilities—if not quite endless—are wide and varied.
“There’s a lot of room for advancement in the advanced practice roles, but I think even for the bedside nurses, there are opportunities. There are so many varieties that people can really find their niche in nursing as a career,” says Dr. Knestrick, who points to her own background as an example.
She started her career practicing for a long-term nursing care facility with a primarily geriatric population. Then she worked in a large tertiary care hospital on a medical-surgical unit, followed by a stint in critical care, before going on to become a nurse manager in pediatric and medical-surgical units, and then teaching in a diploma school of nursing. She has now been a nurse practitioner for 25 years.
Exploring the nursing shortage
Yet although nursing is a high demand, “future proof” field with lots of room for professional growth, the shortage remains a serious issue at present— and is likely to remain so in the future. Says Dr. Knestrick: “According to most of the information I’ve seen about registered nurses, I believe that we’re still going to see a shortage.”
And of course, a shortage of RNs will later translate into a shortage of nurses with more advanced qualifications.
A big part of the problem is that while the aging population may be creating opportunities for healthcare professionals, today’s nursing workforce is also aging.
“The average age of a nurse is around 50,” says Dr. Knestrick. “It’s estimated that over 50% of nurses that are practicing are over the age of 50. This means that within 10 to 20 years they will be retiring from nursing, which will further add to the shortage.”
In fact, the Health Resources and Services Administration predicts more than one million registered nurses will reach retirement age within the next 10 to 15 years, leaving a significant number of jobs to be filled.
This represents not just nurses needing to be replaced, but also a significant loss of knowledge and expertise. As a result, not only do hospitals need to find lots of new nurses, but they need to facilitate the transfer of invaluable nursing wisdom before it is lost.
But here’s another problem: there is also a shortage of nursing teachers to prepare the next generation.
“In some cases, schools have turned down nursing applicants mostly because of the faculty shortage,” says Dr. Knestrick.
What is to be done?
In some states, there are already strategies in place to address the shortage of nurse educators. For instance, the Nurses for Wisconsin initiative provides fellowships and loan forgiveness for future nurse faculty who agree to teach in the state after graduation.
Meanwhile, some nursing schools have formed strategic partnerships to help boost student capacity. For instance, the University of Minnesota has partnered with the Minnesota VA Health Care System to expand enrollment in the schools’ Bachelor’s of Science in Nursing program.
These programs could help with the teaching shortage. But what can employers do?
1) Stress the purpose and potential of a nursing career
In an age when many people are seeking meaningful work, one strategy for attracting new talent is to highlight the social value of nursing and the wide variety of available career paths to candidates.
“They should know that nursing is a wonderful profession,” says Dr. Knestrick, “that there are plenty of opportunities. There will always be sick people and they are always going to need somebody to provide care for them.”
2) Don’t overload nurses
Hospitals seeking cost efficiencies may be tempted to increase the workload on nurses—but this increases the risk of burnout and can make the existing talent shortage worse, says Dr. Knestrick.
A European study of acute care hospitals found that a greater proportion of professional nurses at the bedside is associated with better outcomes for both patients and nurses—thus reducing the risk of staff turnover. So it’s vital to look closely at staffing patterns, and staff accordingly.
3) Talent may be available in other areas
Another option is to recruit nurses from different parts of the country, as demand varies according to geographic areas, says Dr. Knestrick.
Some estimates even project nursing surpluses in some Midwestern states such as Illinois and Minnesota, while states such as California and Colorado will see nursing shortages.
With the correct incentives, it may be possible to target nurses in areas with greater supply and recruit them to areas where demand is more difficult to meet.
4) Make it easier for nurses to acquire—and practice—advanced skills
Employers needing nurses with more advanced qualifications could help provide programs to help them get the masters or doctoral level qualifications needed to become nurse practitioners, says Dr. Knestrick. But there’s another important step, too. Currently, many states place limitations even on nurses with very advanced skills, forbidding them to practice without another healthcare professional in place, thus limiting the extent of the care they can provide their patients.
Many of these rules were written decades ago, says Dr. Knestrick, and don’t reflect current conditions. She recommends that employers “support changes in nurse practice act to remove barriers for nurses, particularly nurse practitioners, to practice to the full extent of their license and their education is essential.”
Of course, enacting these steps and won’t end the nurse shortage immediately, but they are good steps towards ensuring that we don’t run short of these important professionals.
Content courtesy of Indeed
More on bsn jobs


Why Hands-On Experience Matters in Nursing School
Why Hands-On Experience Matters in Nursing School When people think about nursing school, they often picture textbooks, lectures, and exams. While those are important parts…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Sumner College in Bend Meets Nursing Needs
Healthcare in Oregon isn’t just growing—it’s changing. Advances in technology, shifts in patient demographics, and an increased focus on preventative and community-based care are reshaping…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
The Value of a BSN for Oregon’s Growing Healthcare Needs
The Value of a BSN for Oregon’s Growing Healthcare Needs Oregon’s healthcare system is evolving rapidly—and with that growth comes an increasing demand for highly…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Why Earn Your BSN at Sumner College’s Bend Campus
Why Earn Your BSN at Sumner College’s Bend Campus The demand for highly educated nurses continues to grow across the United States. Many healthcare organizations…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
How Advancing Your Degree Expands Your Nursing Career Opportunities
How Advancing Your Degree Expands Your Nursing Career The healthcare industry is constantly evolving, and nurses play a critical role in meeting the growing needs…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
What Employers Look for in New Nursing Graduates in Oregon
Starting Your Nursing Career in Oregon Graduating from nursing school is a major milestone — but what happens next? Healthcare employers in Oregon aren’t just…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Experienced Nursing Faculty & Student Support at Sumner College
If you’re looking for a nursing school in Oregon, choosing the right program means finding experienced instructors and strong academic support. At Sumner College, students…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Nursing In-Demand
Why Nursing Is One of the Most In-Demand Careers Healthcare is an essential industry, and nursing remains one of the most consistently in-demand careers across…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
5 Signs Nursing Might Be the Right Career for You
5 Signs Nursing Might Be the Right Career for You Choosing a career is one of the most important decisions you’ll ever make—and if you’ve…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
From Classroom to Clinic
From Classroom to Clinic: Hands-On Training at Sumner College At Sumner College, education doesn’t stop at the classroom door. From the very first term, students…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
What to Expect Your First Term
Starting college—especially in a healthcare program—is an exciting step, and your first term at Sumner College is designed to set you up for long-term success.…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
How Long Does it Take to Become a Nurse?
How Long Does It Take to Become a Nurse? If you’re considering a career in nursing, one of the first questions you may ask is:…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Why Should I Pursue a BSN Degree?
Why Should I Pursue a BSN Degree? | Benefits of Earning Your Bachelor of Science in Nursing If you’re exploring a career in nursing or…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Become a LPN Today!
Do I Need an Undergraduate Degree to Be a Nurse? If you’ve ever thought about becoming a nurse, you might assume it requires a four-year…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Honoring Service – How Military Experience Translates to a Career in Healthcare
At Sumner College, we proudly honor our veterans and active-duty service members this Veterans Day Weekend. Service in the military is built on dedication, teamwork,…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Future nurses—don’t forget!
Your TEAS exam is one of the most important steps in your Sumner College application process! The TEAS (Test of Essential Academic Skills) helps measure…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Sumner College Partners with K103 for the 2024 Holiday Toy Drive – Donations Now Open!
The holiday season is officially underway, and Sumner College is excited to announce our partnership with K103’s Annual Holiday Toy Drive, launching today! This joyful…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Why Should I Pursue a BSN Degree?
Thinking about advancing your nursing education? Earning your Bachelor of Science in Nursing (BSN) is one of the best investments you can make in your nursing career—and in…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
What Is a BS in Nursing?
If you’re a registered nurse looking to take your career to the next level, you’ve probably heard about earning your BS in Nursing (BSN). But what…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
What Prerequisites Do I Need For a Nursing Degree?
Dreaming of becoming a nurse but worried about all the prerequisites? At Sumner College, we’ve removed the biggest roadblock to your nursing education — no…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Sumner College Ranked #3 in Best Value Colleges in Oregon
At Sumner College, our mission has always been to provide high-quality nursing education that’s both accessible and affordable. We’re proud to share that Sumner College…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
FAFSA Season
The vast majority of college students—more than 85%—rely on financial aid to make higher education possible. At the center of that process is the Free…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
How Many Years Does It Take To Get A Nursing Degree?
How Many Years Does It Take to Get a Nursing Degree? If you’re thinking about a career in nursing, one of the first questions that…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
All About CCNE Accreditation
Why CCNE Accreditation Matters – And What It Means for Sumner College Students When choosing a nursing program, one of the most important factors to…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Is There a 2 Year Nursing Degree?
Is There a 2-Year Nursing Degree in the United States? If you’re considering a career in nursing, you’ve probably wondered about the different educational pathways…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Why Should I Get a BSN?
Why Should I Get a BS in Nursing? If you’re considering a career in healthcare, you may already know that nursing is one of the…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Become a Registered Nurse in Less Time with Sumner College
Become a Registered Nurse in Less Time with Sumner College For many people who feel called to nursing, the idea of spending four or more…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Nursing at Sumner College
Becoming a Nurse: Your Path Starts at Sumner College Nursing is more than a career—it’s a calling. Nurses are at the heart of healthcare, providing…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Is it Hard to Get Your First Nursing Job?
Is it Hard to Get Your First Nursing Job? Starting your career in nursing is an exciting and meaningful step—but for many recent graduates, the…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
What is CCNE Accreditation?
When researching nursing schools, you may come across the term CCNE accreditation. But what does it really mean—and why is it so important for your…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn