Practical Nursing Program
Follow Your Passion and Become a Nurse
Request Information
Practical Nursing
PRACTICAL NURSING
The Practical Nursing Program at Sumner College can fast-track you to a new career as an LPN in just 13 months. If you are compassionate about others and want to make a difference in the field of healthcare, Sumner College may be the right choice for you.
What sets us apart? Let’s start with small class sizes, exceptional clinical opportunities, and employer partnerships that hire over 72% of our students at facilities where they complete their capstone clinical experience. Quarterly Career Fairs and our own Sumner College Medical Club allow students the opportunity to network with employers while attending school.
According to the Oregon State Board of Nursing, 40% of Oregon’s PN graduates who sat for the NCLEX were from Sumner College. Source: https://www.oregon.gov/osbn/Documents/Resource_NCLEXPassrates.pdf
We also provide every student in the program with a Lenovo laptop computer and the support services that foster student success. With a 97% retention rate for the current reporting year, we know what it takes to help that Dream of becoming a nurse a reality for our students.
Ready to take the next step? Download an Information Packet and contact us to set up a tour today!
Classes start every 10 weeks.
WHAT SETS US APART?
- New Term Every 10 Weeks
- 13 Month Program
- 97% Program Retention
- Over 100 Clinical Sites
- 24 Students: Average Class Size
Our Program
PRACTICAL NURSING
Sumner College is committed to providing a strong foundation for our students who are committed to excellence and prepared to begin their journey in a career that provides professional growth and advancement opportunities, while truly making a difference in people’s lives.
Our program embraces the mission of delivering high quality instruction in classroom, skills lab, and clinical settings that ensure students are equipped with the knowledge needed to contribute to the profession and the health care needs of the community.
This program allows students the opportunity to enter into a nursing program without completing prerequisite courses, and term schedules are set up by the college to assure students who complete all of the required courses can graduate in just over a year.
The Practical Nursing Program at Sumner College is approved by the Oregon State Board of Nursing (OSBN) and the Department of Education. We are authorized by the Office of Degree Authorization (ODA) to award diplomas and degrees, and accredited by the Accrediting Bureau of Health Education Schools (ABHES).
If your Dream includes advancing your practice in the future, we’ve got options for you to consider.
Dream It. Do It. At Sumner College.
PROGRAM INFORMATION
- Application Fee: $50
- Registration Fee: $100
- Lab and Technology Fee: $2,600
- Program Tuition: $33,975
Total Cost of Program: $36,725
Book an Accuplacer Exam:
Book an LPN Info Session
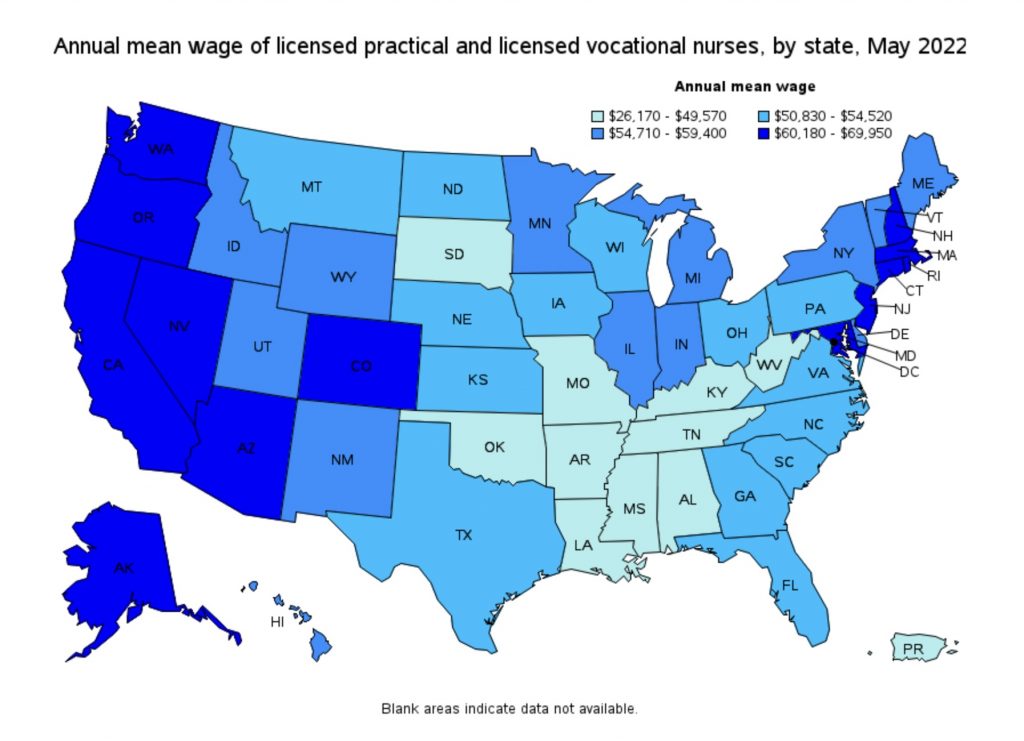
Career Outlook
NURSING CAREER
The field of nursing is an occupation that has continued to grow on an annual basis. According to the Bureau of Labor Statistics, employment of licensed practical nurses is projected to grow 11 percent from 2018-2028, much faster than average for all occupations. As the baby-boomer population ages, the overall need for healthcare services is expected to rise. That age demographic, as well as many procedures that used to require a hospital visit now being done outside of hospitals, creates a demand in other settings such as outpatient care centers.
The average median starting salary of our own graduates during the 2023-2024 reporting year was $34.00 per hour.
Where Grads Work
- US Dept of Veteran’s Affairs
- Sono Bello
- Prestige Care
- Avamere
- Vibra Specialty Hospital
- Fresenius Medical Care
- Marquis Companies
- Naphcare
- Action Healthcare
- Clackamas County Corrections
- Columbia River Mental Health
- Fort Vancouver Acute Care
- Frontier Rehab & Extended Care
- The Children’s Clinic
- Vancouver Clinic
- Beacon Bill Rehabilitation
- Columbia Asthma & Allergy
- Hampton and Ashley Inn
- Brookdale Senior Living
- Regency Gresham
- Mirabella
- Washougal School District
- Cascade Park Care Center
- Trilogy Home Center
To find out more about our program, download the Program in Nursing Information kit below and reserve a seat to attend an upcoming Information Session.
13 Months to A New Career
Learn more:
Why Sumner College
- No prerequisites required to apply
- Program designed to be completed in 13 months
- Small lab classes provide individual attention and support
- Graduates are prepared to sit for the NCLEX-PN exam
- Program starts new cohorts every 10 weeks
- Financial Aid for those who qualify
- Hands-on program promotes strong critical thinking skills
- Offering career-focused education since 1974
- 97% Program Retention -2021-2022 reporting statistics annualized
- Over 100 Clinical Sites offer a broad range of learning experiences
- College grants awarded based on academics and attendance
- Career Services Department assists in career placement after graduation

Traci F.
LPN | Charge Nurse & Preceptor
“...if somebody wants to make a career change but is hesitant, I would encourage them to GO FOR IT!”
Read Full Spotlight










Sumner College in Bend Meets Nursing Needs
Healthcare in Oregon isn’t just growing—it’s changing. Advances in technology, shifts in patient demographics, and an increased focus on preventative and community-based care are reshaping…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
The Value of a BSN for Oregon’s Growing Healthcare Needs
The Value of a BSN for Oregon’s Growing Healthcare Needs Oregon’s healthcare system is evolving rapidly—and with that growth comes an increasing demand for highly…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Why Earn Your BSN at Sumner College’s Bend Campus
Why Earn Your BSN at Sumner College’s Bend Campus The demand for highly educated nurses continues to grow across the United States. Many healthcare organizations…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
How Advancing Your Degree Expands Your Nursing Career Opportunities
How Advancing Your Degree Expands Your Nursing Career The healthcare industry is constantly evolving, and nurses play a critical role in meeting the growing needs…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
What Employers Look for in New Nursing Graduates in Oregon
Starting Your Nursing Career in Oregon Graduating from nursing school is a major milestone — but what happens next? Healthcare employers in Oregon aren’t just…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Experienced Nursing Faculty & Student Support at Sumner College
If you’re looking for a nursing school in Oregon, choosing the right program means finding experienced instructors and strong academic support. At Sumner College, students…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Nursing In-Demand
Why Nursing Is One of the Most In-Demand Careers Healthcare is an essential industry, and nursing remains one of the most consistently in-demand careers across…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
5 Signs Nursing Might Be the Right Career for You
5 Signs Nursing Might Be the Right Career for You Choosing a career is one of the most important decisions you’ll ever make—and if you’ve…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
From Classroom to Clinic
From Classroom to Clinic: Hands-On Training at Sumner College At Sumner College, education doesn’t stop at the classroom door. From the very first term, students…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
What to Expect Your First Term
Starting college—especially in a healthcare program—is an exciting step, and your first term at Sumner College is designed to set you up for long-term success.…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
How Long Does it Take to Become a Nurse?
How Long Does It Take to Become a Nurse? If you’re considering a career in nursing, one of the first questions you may ask is:…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Why Should I Pursue a BSN Degree?
Why Should I Pursue a BSN Degree? | Benefits of Earning Your Bachelor of Science in Nursing If you’re exploring a career in nursing or…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Become a LPN Today!
Do I Need an Undergraduate Degree to Be a Nurse? If you’ve ever thought about becoming a nurse, you might assume it requires a four-year…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Honoring Service – How Military Experience Translates to a Career in Healthcare
At Sumner College, we proudly honor our veterans and active-duty service members this Veterans Day Weekend. Service in the military is built on dedication, teamwork,…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Future nurses—don’t forget!
Your TEAS exam is one of the most important steps in your Sumner College application process! The TEAS (Test of Essential Academic Skills) helps measure…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Sumner College Partners with K103 for the 2024 Holiday Toy Drive – Donations Now Open!
The holiday season is officially underway, and Sumner College is excited to announce our partnership with K103’s Annual Holiday Toy Drive, launching today! This joyful…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Why Should I Pursue a BSN Degree?
Thinking about advancing your nursing education? Earning your Bachelor of Science in Nursing (BSN) is one of the best investments you can make in your nursing career—and in…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
What Is a BS in Nursing?
If you’re a registered nurse looking to take your career to the next level, you’ve probably heard about earning your BS in Nursing (BSN). But what…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
What Prerequisites Do I Need For a Nursing Degree?
Dreaming of becoming a nurse but worried about all the prerequisites? At Sumner College, we’ve removed the biggest roadblock to your nursing education — no…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Sumner College Ranked #3 in Best Value Colleges in Oregon
At Sumner College, our mission has always been to provide high-quality nursing education that’s both accessible and affordable. We’re proud to share that Sumner College…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
FAFSA Season
The vast majority of college students—more than 85%—rely on financial aid to make higher education possible. At the center of that process is the Free…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
How Many Years Does It Take To Get A Nursing Degree?
How Many Years Does It Take to Get a Nursing Degree? If you’re thinking about a career in nursing, one of the first questions that…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
All About CCNE Accreditation
Why CCNE Accreditation Matters – And What It Means for Sumner College Students When choosing a nursing program, one of the most important factors to…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Is There a 2 Year Nursing Degree?
Is There a 2-Year Nursing Degree in the United States? If you’re considering a career in nursing, you’ve probably wondered about the different educational pathways…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Why Should I Get a BSN?
Why Should I Get a BS in Nursing? If you’re considering a career in healthcare, you may already know that nursing is one of the…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Become a Registered Nurse in Less Time with Sumner College
Become a Registered Nurse in Less Time with Sumner College For many people who feel called to nursing, the idea of spending four or more…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Nursing at Sumner College
Becoming a Nurse: Your Path Starts at Sumner College Nursing is more than a career—it’s a calling. Nurses are at the heart of healthcare, providing…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
Is it Hard to Get Your First Nursing Job?
Is it Hard to Get Your First Nursing Job? Starting your career in nursing is an exciting and meaningful step—but for many recent graduates, the…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
What is CCNE Accreditation?
When researching nursing schools, you may come across the term CCNE accreditation. But what does it really mean—and why is it so important for your…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn
LPN V.S. BSN at Sumner College
Understanding the Difference Between LPN, RN, and BSN — and How Sumner College Can Help You Get There When considering a career in nursing, it's…
Share at FacebookShare at TwitterShare at PinterestShare at LinkedIn